Stop googling your medical symptoms and diagnosis/mayo stop googling your medical symptoms and signs stop googling your medical records stop googling your medical group stop googling your medical rights stop googling let s talk by sherry turkle stop googling people stop googling colon cancer

Stop Googling your medical symptoms and do this instead
Diagnosing yourself online is a slippery slope. You could Google "why do I have pain in my ribs" and come away with the possibility that you have a pinched nerve (possible) or fatal internal bleeding (unlikely, unless you've been impaled).
You should certainly know how to take care of yourself in the case of a common cold, migraine, or other relatively benign condition, and online health information can help you make the right decisions when you actually know what condition you have.
The problem is, the internet might make you think that a common cold is a bacterial infection (it's a virus, which won't respond to antibiotics), that a migraine is a brain tumor or an aneurysm and that an abdominal cramp is appendicitis.
In fact, research suggests that online symptom checkers are almost always wrong. So before you spiral down the symptom rabbit hole, learn why obsessively Googling symptoms is risky and how to look for accurate health information online.
Why you should avoid over-Googling your symptoms
There are essentially two bad ways this can go: Either you overestimate your symptoms and end up taking the wrong medication or engaging in the wrong self-treatment, or you underestimate your symptoms and let a condition worsen.
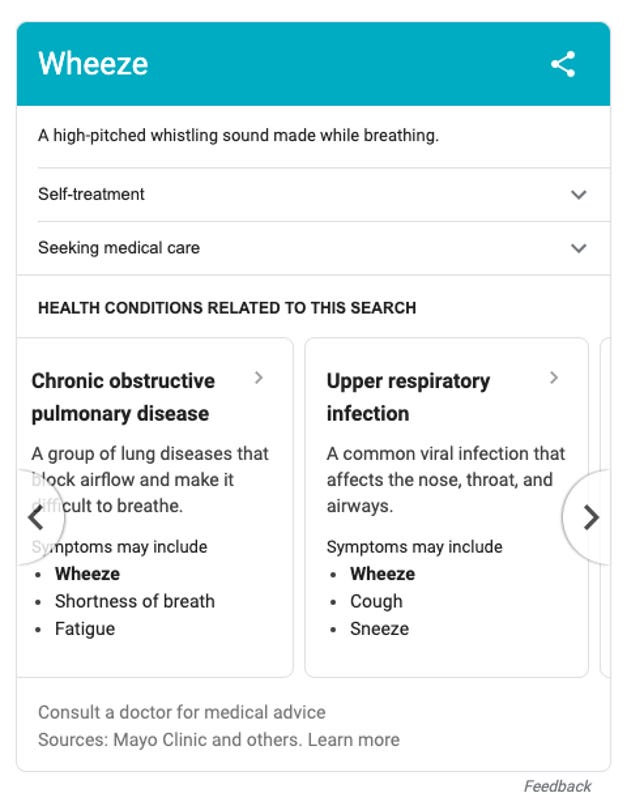
Google provides medical information for common conditions, but it's still always best to see a doctor.
Screenshot by Sarah Mitroff/CNETThere's also the risk of developing "health anxiety," real condition that involves excessive worrying that you are sick. You may know this condition as hypochondriasis, and you're probably familiar with the word "hypochondriac."
Even if you're not a hypochondriac, searching for medical symptoms and illnesses online may add unnecessary worry and a lack of peace of mind to your life. The internet-age term for this is "cyberchondria."
Research notes that while internet information can help people avoid unnecessary doctor visits for minor (or nonexistent) conditions, some people feel anxiety and fear about medical information they find online.
Part of the reason that searching for symptoms can send you into an anxious spiral has to do with the fact that there's just so much health information online. While a great deal of online health content is trustworthy and accurate, much of it is not. But you can learn to decipher the good from the bad with the right tips.
Tips for finding accurate health content online
If you must search your symptoms, make sure to weed out questionable content by following these guidelines.
If you're reading lay media
- Look for articles that back up their claims by linking out to or citing peer-reviewed clinical studies. For example, an article that says "eating too much sugar may increase your risk for depression" should link to a primary source that says so, like this one.
- Whenever possible, read the full report or abstract of those peer-reviewed clinic studies and look for the conclusion to verify the results of the study.
- Articles that quote experts or are written by topic area experts (or both) are also usually reliable. An article titled "5 things that happen to your body when you drastically cut carbs" is likely to be way more trustworthy when it includes insight from a nutrition professional or is written by a nutrition professional.
- If an article doesn't include expert insights or isn't written by a topic area expert, check to see if it was reviewed by an appropriate health professional. Many health publishers now have review boards that consist of topic area experts who ensure content accuracy. For example, this piece about Crohn's Disease on Healthline was reviewed by a medical doctor.
- Search for the publisher's health editorial policy. Many health publishers have these policies available on their websites, and it's a good sign when they do. It means the publisher has strict editorial guidelines when it comes to writing health content and citing experts or primary sources.

Look for articles that were reviewed by a doctor or medical professional.
Screenshot by Sarah Mitroff/CNETIf you're reading primary sources
First, the definition of a primary source: A primary source is a firsthand account of a topic or event. When it comes to health and science, primary sources refer to documents that provide the full account of the original research. In other words, the actual research articles published in scientific journals, such as The Journal of Neuroscience or the Journal of Food Science and Technology. The best place to find these articles is on PubMed, a resource provided by the National Institutes of Health's US National Library of Medicine.
When reading articles from scientific journals, keep these considerations in mind:
- Look for author affiliations and conflicts of interest. Anytime a scientist partakes in a research study or writes a scientific article, they must declare their affiliations and potential conflicts of interest so that any bias is disclosed. For example, an article about cryotherapy that was partially written by someone affiliated with a cryotherapy wholesaler would present a conflict of interest.
- Look for commissioning and funding information. Just like author affiliations and conflicts, commissioning and funding information must be disclosed in the name of bias. Many companies in the health industry commission and fund research studies to prove the efficacy of their products. That's totally fine -- it doesn't necessarily mean the results are skewed -- but just know that company-funded studies are not independent, third-party studies, which are the most reliable.
- Check to see if the study has been cited in other studies. Since there's so much research out there, scientists often use existing research articles as sources for new research articles. It's not a bad sign if an article hasn't been cited by other articles, but it's definitely a good sign if it's been cited many times. Most research articles have a "cited by [number]" callout online.
- Check the date. Science -- particularly nutrition and medical science -- evolves quickly. Look for studies no older than 10 years, but preferably no older than five years, if you're looking for answers about a condition or symptoms you currently have.
When the internet fails, see a doctor
If even after scouring through research you still feel lost, just go see your doctor. Not everyone can be a doctor -- and the internet certainly cannot -- so give yourself the luxury of peace of mind by seeing a real health professional.
And if carving out time for an in-person doctor's appointment isn't an option, try seeing a doctor online via one of the many telehealth companies. You can also talk to a therapist online if your worries sit more in the realm of mental or emotional health.
The information contained in this article is for educational and informational purposes only and is not intended as health or medical advice. Always consult a physician or other qualified health provider regarding any questions you may have about a medical condition or health objectives.
The information contained in this article is for educational and informational purposes only and is not intended as health or medical advice. Always consult a physician or other qualified health provider regarding any questions you may have about a medical condition or health objectives.
Source